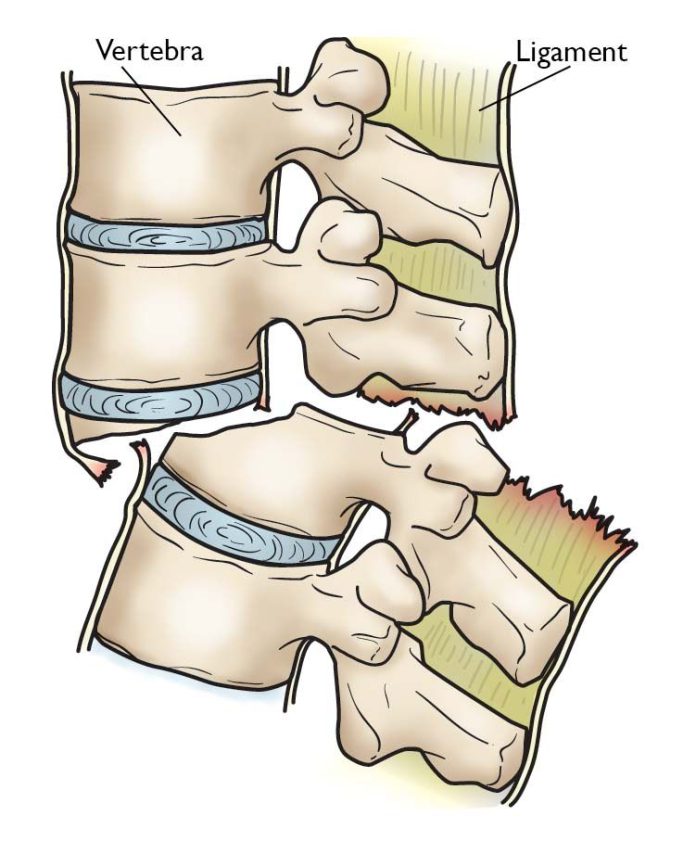
Ngumpi.com – During an automobile accident, the most common mechanism for distracting injuries is seatbelts. These injuries typically involve the spine’s posterior segments, which can become severely disrupted. Magerl et al. classified thoracolumbar flexion-distraction injuries as B1 and B2.
The results of this procedure should be evaluated by a certified spinal surgeon
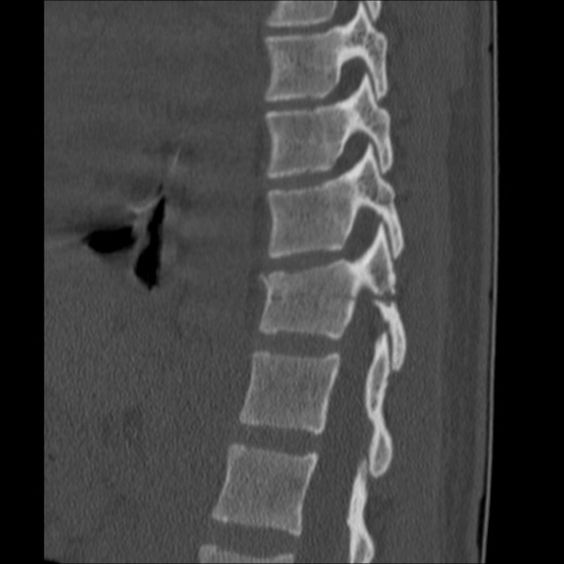
In addition to apical dislocation, fractures of the B1.1.1 and B2.1 vertebrae can be caused by the transverse ligament. The investigator should rule out possible rotational offset within the vertebral segments, which is a sign of an instable type C fracture. In these cases, the surgeon may perform a percutaneous fixation of the fracture. However, the results of this procedure should be evaluated by a board-certified spine surgeon.
A physical examination should begin immediately after airway stabilization, and should include a neurologic examination. Palpation is crucial in identifying associated spinal injuries. Transverse band of ecchymosis suggests flexion-distraction injury, while bruising along the rib cage is indicative of a thoracic fracture. In addition, spontaneous pain in the spine should be noted if local hematomas are present. The spine should be palpated for tenderness, step-off, or interspinous process gapping.
The purpose of spinal trauma diagnostics
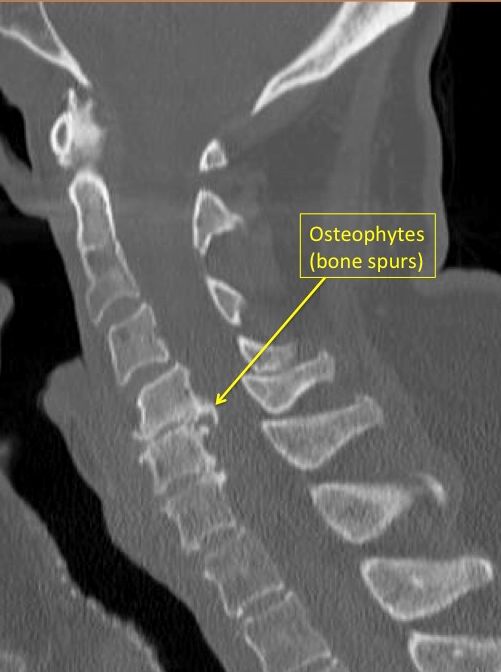
An MRI is not a suitable imaging tool for polytrauma diagnosis. In addition, its long exam time and limited intervention opportunities inside the apparatus limit its utility in treating spinal trauma. Damage control principles do not favor diagnostic delays. A rapid stabilization is preferred. The goal of spinal trauma diagnostics is to stabilize the patient. While a patient can still be unconscious, MRI does not provide the necessary information to diagnose the condition.
In vitro experiments with large load rates create an unstable spinal unit. This makes the spine more likely to become unstable after trauma, so it is crucial to test the effects of different loading rates. The study design should account for varying degrees of deformation in all spinal units and combine the different types of load. In this way, distraction-distraction trauma can be safely simulated in a laboratory. And as long as the biomechanical response is intact, it is a valuable tool for diagnosis.
The most common trauma mechanism involves sternal fixation
In addition to evaluating sternal fractures, a recent study evaluated patients who had sustained both a spinal and a sternal fracture. Twenty-seven of these patients recovered without neurologic deficits and did not complain of pain at follow-up. The most common trauma mechanisms involved sternal fixation, including road traffic accidents, falls from a height, and a debris avalanche.
Ultimately, the treatment of the patient with spinal injury should balance the need for stabilization with the reduction of iatrogenic secondary trauma. The best approach is to assess the spine and damage control before deciding on a course of action. By doing so, patients will benefit from an early diagnosis and appropriate treatment. This will prevent unnecessary complications and reduce iatrogenic trauma. However, complications and surgical procedures may arise. In these situations, early total care is crucial to prevent further complications.
Open reduction is preferred if the fracture is rotationally unstable

Patients with fractures of the vertebral column and spine should undergo open reduction and posterior instrumentation. Open reduction is preferred when the fractures are rotationally instable. This will limit the chances of second hits. If the patient undergoes a second trauma, surgery should be performed on the anterior portion. It is imperative that a patient’s immune system is restored before anterior surgery is performed. The patient must undergo rehabilitation.
Neurologic examination is also important in assessing whether traction is effective in treating the patient’s condition. This assessment should include assessment of the presence of perianal sensation, voluntary contraction, and bulbocavernosus reflex. The American Spinal Injury Association has established a useful template for neurologic examination. It includes light touch and pinprick sensations in 28 dermatomes. These factors help assess whether the patient is suffering from neurologic injury.